16 Disease of the Right Ventricle
16.1 Introduction
Assessment of the right heart is an important part of every exam. It enables the investigator to diagnose diseases of the right heart as well as provides crucial information to better understand the sequelae of left heart disease. The right ventricle is closely related to many diseases of the left ventricle.
In Chapter 2 we described visualization of the right ventricle by means of echocardiography. Right ventricular anatomy, its function, and methods of quantification were described in Chapter 3. In this section we will focus on various conditions and diseases that involve or affect the right ventricle. We will address right ventricular pressure overload (i.e. pulmonary hypertension), volume overload (i.e. tricuspid regurgitation, atrial septal defects), and dysfunction of the right ventricular myocardium as it occurs in right heart infarction and right ventricular dysplasia.
16.2 Pulmonary hypertension
16.2.1 Pathophysiology of pulmonary hypertension
Pulmonary hypertension is defined as an increase in mean pulmonary pressure to a level higher than 25 mmHg (normal = 14±3 mmHg) at rest.
Exercise-induced pulmonary hypertension (>30 mmHg) is currently not included in the definition of pulmonary hypertension.
Pulmonary hypertension may occur in several conditions. Differentiating between these requires the use of several imaging modalities (CT scan, pulmonary scintigraphy, echocardiography), laboratory data, and specifically right heart catheterization. The following groups of conditions and individual conditions may cause pulmonary hypertension:
- Pulmonary arterial hypertension (PAH)
- Pulmonary hypertension due to left heart disease
- Pulmonary veno-occlusive disease
- Pulmonary hypertension due to lung disease and hypoxia
- Chronic thromboembolic pulmonary hypertension (CTEPH)
- Pulmonary hypertension due to ambiguous or multifactorial mechanisms
1. Pulmonary arterial hypertension (PAH)
1.1. Idiopathic PAH
1.2. Inherited
1.2.1. BMPR2
1.2.2. ALK1, endoglin (with or without hemorrhagic teleangiectasia)
1.2.3. Unknown
1.3. Drug- or toxin-induced
1.4. Associated with
1.4.1. Connective tissue disease
1.4.3. HIV infection
1.4.3. Portal hypertension
1.4.4. Congenital heart disease
1.4.5. Schistosomiasis
1.4.6. Chronic hemolytic anemia
1.5. Persistent pulmonary hypertension of the newborn
1‘. Pulmonary veno-occlusive disease (PVOD) and/or pulmonary capillary hemangiomatosis (PCH)
2. Pulmonary hypertension due to left heart disease
2.1.Systolic dysfunction
2.2. Diastolic dysfunction
2.3. Valvular disease
3. Pulmonary hypertension due to lung disease and/or hypoxia
3.1. Chronic obstructive pulmonary disease
3.2. Interstitial lung disease
3.3. Other pulmonary diseasse with a mixed restrictive and obstructive pattern
3.4. Sleep-disordered breathing
3.5. Alveolar hypoventilation disorders
3.6. Chronic exposure to high altitudes
3.7. Developmental abnormalities
4. Chronic thromboembolic pulmonary hypertension (CTEPH)
5. Pulmonary hypertension with ambiguous multifactorial mechanisms
5.1. Hematologic disorders: myeloproliferative disorders, splenectomy
5.2. Systemic disorders: sarcoidosis, pulmonary Langerhans cell histiocytosis, lymphangioleiomyomatosis, neurofibromatosis, vasculitis
5.3. Metabolic disorders: glycogen storage disease, Gaucher's disease, thyroid disorders
5.4. Others: tumoral obstruction, fibrosing mediastinitis, chronic renal failure on dialysis
The following diagram shows how frequently pulmonary hypertension is caused by the individual forms. Clearly, left heart disease is by far the most common cause of pulmonary hypertension.
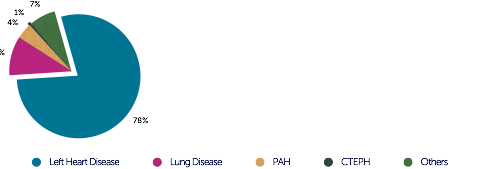
In left heart disease, pulmonary hypertension is characterized by elevated left ventricular filling pressures, which translate into the pulmonary circulation. Therefore, it is also known as "post-capillary" pulmonary hypertension. In contrast, all other forms of pulmonary hypertension are characterized by elevated pulmonary vascular resistance (> 3 Wood units/ > 240 dyn*s*cm-5). Left ventricular filling pressures are normal or just mildly elevated (pulmonary capillary wedge pressure < 15 mmHg). These forms are referred to as pre-capillary hypertension. Although echocardiography is very important to determine whether left heart disease is present, a clear distinction between pre- and post-capillary hypertension is not always achieved with echocardiography; invasive pressure measurements are required. By determining pressure in the left heart (left ventricular end-diastolic pressure) or obtaining an indirect estimation of left ventricular filling pressures (pulmonary wedge pressure) it will be possible to determine the presence of pre- or post-capillary pressure. In addition, it permits calculation of pulmonary vascular resistance, cardiac output, as well as detection and quantification of shunts.
Diastolic dysfunction is an important cause of pulmonary hypertension. The patients occasionally present with significant pulmonary hypertension, an enlarged left atrium, and severe tricuspid regurgitation. Some patients have a severely elevated PA pressure and moderately increased left-sided filling pressure. This condition is referred to as "out-of-proportion" pulmonary hypertension. Severe pulmonary hypertension is rare in chronic obstructive pulmonary disease.In general, the right ventricle reacts in terms of dilatation, right ventricular hypertrophy and eventually right heart failure. The degree of abnormalities depends on the severity of pulmonary hypertension and how rapidly it develops. When it develops slowly the right ventricle has time to adapt and is able to cope with the increase in right ventricular afterload. The final stage of the disease is typically marked by severely reduced right ventricular function and a low cardiac output. Since the right ventricle is "coupled" with the left one, left ventricular function may also be disturbed. In the following sections you will learn about morphological abnormalities seen on echocardiography.
