Dying Hearts
In echocardiography we are able to observe the heart from the first to the last beat of our lives. In one of the recent blog articles we showed you a beating heart in very early life: that of a fetus. We now turn to the final moments of life - the moments when the heart struggles with death. As tragic and dramatic as this event is, it does provide important information that helps us to understand the pathophysiology of the heart and how we should treat a patient.
Struggle for cardiac output
I suppose every heart looks a little different at the end of one's life. It depends on the underlying disease. Many hearts just beat slower and slower until electromechanical dissociation occurs. The following heart is that of a patient with end-stage heart failure. It was an 88-year-old man with dilated cardiomyopathy, who received all the treatment we were able to provide, including a CRT-ICD system.
 Very poor left ventricular function in end-stage heart failure.
Very poor left ventricular function in end-stage heart failure.
His cardiac function is very poor. The heart is trying to compensate by increasing heart rate. The patient clearly had pulmonary edema despite high-dose diuretics. His blood pressure was starting to drop. Look at the PW Doppler signal across the LVOT.
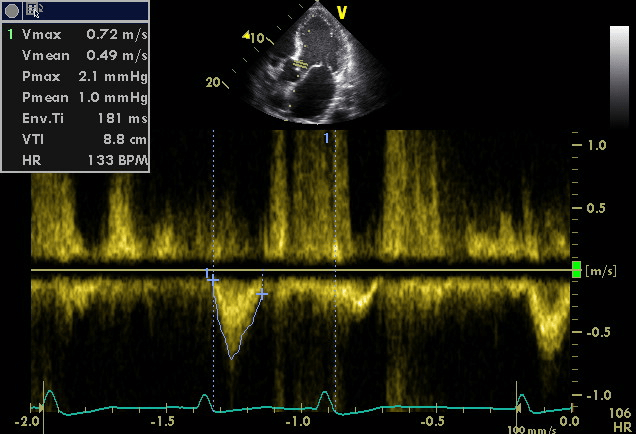 Low cardiac output in a dying heart.
Low cardiac output in a dying heart.
The velocity time integral is very low (8.8 cm). His cardiac output is too low to sustain organ function. At the time his lactate levels were rising steadily. He died just 30 minutes later.
Much too fast
Other critical moments may also cause a very low cardiac output. We investigated the following patient who had coronary artery disease and normal left ventricular function. All of a sudden he developed ventricular tachycardia with a very high heart rate.
 Ventricular tachycardia during echocardiography.
Ventricular tachycardia during echocardiography.
When you see this image it becomes quite obvious that ventricular tachycardia is a life-threatening situation. Note how small the ventricle is. There is little time for filling and the atria are contracting against the ventricles (AV dissociation). On this long-axis view one can hardly see the aortic valve open. Our patient was fortunate. We started resuscitation and performed cardioversion, and he survived. Luckily we were there at the time and established the diagnosis even before we had the time to perform a full 12-lead ECG.
Why chest compression works
The next patient will clearly show you why cardiac compression is a crucial aspect of resuscitation. This case also shows you how valuable echocardiography is in this setting.
A 45-year old man returned from the operating room after bypass surgery. His blood pressure started to drop and he developed ST elevations in the inferior leads. A TEE probe was inserted at the time. See what happened all of a sudden:
 Cardiac arrest documented with transesophageal echocardiography.
Cardiac arrest documented with transesophageal echocardiography.
The patient developed cardiac arrest. Note how the mitral valve fibrillates but there is no contractile function of the heart. The information provided by echo is extremely valuable, isn't it? It is easy to determine whether a TRUE cardiac arrest is present. The value of echocardiography is now well appreciated in the field of emergency medicine. It's an integral aspect of advanced life support in helping to distinguish between various causes of pulseless electrical activity. The next case shows stasis of blood. Within seconds we see “sludge” in the heart. Can you see what was done next?
 TEE study showing the effects of chest compression.
TEE study showing the effects of chest compression.
Chest compression was started. Note that the right and the left ventricles are compressed and blood is starting to circulate. The mitral vale opens and closes again and the sludge in the left ventricle vanishes. Is this not a very lucid demonstration of the importance of chest compression? This patient was also fortunate. After electric cardioversion of subsequent ventricular fibrillation and under appropriate medical treatment including extracorporeal membrane oxygenation, we were able to achieve a stable rhythm:
 TEE study shortly after cardioversion.
TEE study shortly after cardioversion.
His function - especially right ventricular function - has still not returned to normal. This is caused by the underlying problem....he had acute graft closure of the RCA bypass, which is the vessel that also supplies the right ventricle, and therefore underwent immediate re-operation.
Value of echo in dying hearts
Three examples of different critical situations. Situations that did- or could - end the life of a patient. How did echo help in these three settings? Once we noted the first patient's poor left ventricular function and realized he did not have any options, we called in for the family to be with him during his final moments. In the second patient we found that a rhythm problem was present (with echo!) and immediately initiated therapy. Finally, in the third patient we were able to not only establish the diagnosis of cardiac arrest but also identify the problem and monitor the effects of resuscitation.
So echo does make a difference. Join our Master's class if you have not done so yet, and learn echocardiography from your mentors. You will see the difference!
Best
Thomas & Georg



